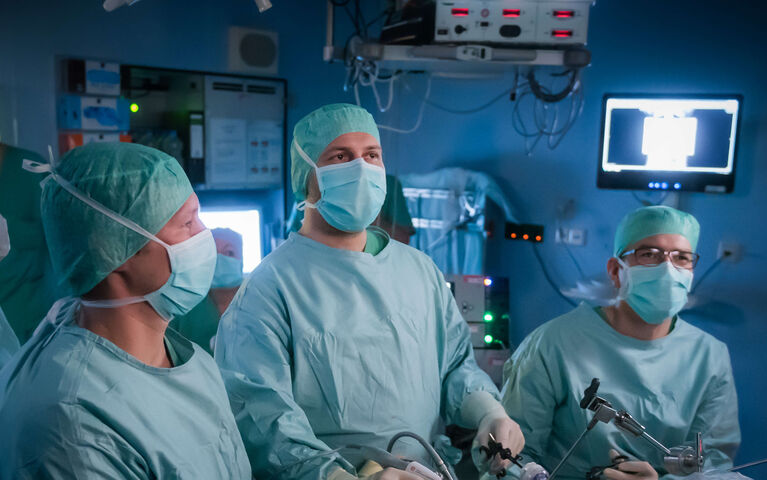
Bariatric Surgery
At the recognized Center of Excellence for Minimally-Invasive and Bariatric Surgery
At a glance
Weight loss surgery (bariatric surgery) is performed with great expertise by the extremely experienced surgeons of our Section for Minimally Invasive and Bariatric Surgery at Heidelberg Department of Surgery. There are various options available for patients desiring surgery for weight loss and to improve comorbidities, especially type 2 diabetes mellitus, in Germany:
- Gastric sleeve surgery
- Gastric bypass
- Single-anastomosis duodeno-ileal bypass with sleeve (SADI-S)
- Duodenal switch
- Gastric balloon
- Gastric band
In most cases, gastric sleeve surgery and gastric bypass are recommended. The best option for each patient is discussed individually.
-

Our hospital has been recognized as a center of excellence for minimally invasive surgery, because we have exceptional experience and state-of-the-art operating facilities. Thus, we can offer patients very safe and effective bariatric surgery that can help them lose significant amounts of weight and achieve better health and quality of life.
Our Specialists
Bariatric Surgery - Why and when?
Prerequisites for surgery:
- Moderate to High-Risk Obesity (BMI > 35) and
- Severe secondary consequences / comorbidities, especially type 2 diabetes mellitus
Obesity is a condition associated with many other medical problems like type 2 diabetes mellitus, high blood pressure, fatty liver, dyslipidemia, and others. Quality of life is markedly decreased. Most therapies, such as diets, do not lead to sustained weight loss. If patients have already been unsuccessful with these therapies, surgery can be a reasonable next step.
Benefits of bariatric surgery for most patients:
- Long-term weight loss - most patients lose approximately 60-80% of overweight within 2 years
- Long-term increase in quality of life
- Decline of type 2 diabetes mellitus
- Significant improvement of comorbidities (e.g. hypertension, fatty liver, dyslipidemia, sleep apnea)
Further benefits
For patients with type 2 diabetes mellitus
- Diabetes mellitus often resolves within a few days to weeks after surgery and patients often need less or no medications any more.
- The occurrence of diabetic complications such as kidney damage up to a need for dialysis, heart attack, or amputations and even existing complications are markedly reduced.
- The effects of bariatric surgery on type 2 diabetes mellitus or fatty liver are unrelated to initial BMI. This means that surgery has the same effect on slightly obese diabetics as on severely obese patients.
- As a result, bariatric surgery can prolong the life of affected patients.
Further information: Surgery
Bariatric surgery options
In Heidelberg as well as internationally, gastric sleeve surgery and gastric bypass surgery are generally performed. Both procedures result in the same weight loss and have similar effects on diabetes and other comorbidities. Both of these operations will leave patients needing lifelong vitamin and trace element replacement.
Gastric sleeve
During the gastric sleeve procedure, two thirds of the stomach is removed and with it, hormone-active cells responsible for the feeling of hunger. With the removal of these cells and the reduction of stomach size, various changes in second messengers and metabolic processes are triggered and the patient's food intake per meal is significantly reduced. The gastric sleeve is considered a technically simple, safe and effective procedure.
Gastric Bypass
During gastric bypass, the stomach is divided so that food only reaches the upper part (the vestibule), which produces a rapid satiety signal. The remaining partially-digested food then bypasses the rest of the stomach through a loop of small intestine. This re-routing triggers various changes in the second messengers and metabolic processes and the body absorbs fewer nutrients. Weight is reduced, thus also improving the comorbidities. This surgery has shown good long-term success.
If possible, these operations are performed with a minimally invasive approach.
The Duodenal switch procedure, gastric balloon (for BMI > 60) or gastric bands (gastric band - especially for adolescent patients under 18 years) are used only in special cases.
What are the risks?
Both common procedures are extremely safe in experienced hands, with complication rates under 2%.
Nevertheless as with all operations, complications can occur, such as suture leakage, bleeding, infection, allergic reactions to anesthesia, cardiovascular reactions, and more. Complications that do occur are well controlled in most cases thanks to much experience with large abdominal surgeries that are commonly performed in our center.
In the medium and long-term, there are particular problems affecting digestion such as nausea, diarrhea, constipation, low blood sugar or ulcers.
All risks are discussed in detail with each patient prior to surgery, and there's an opportunity to address all questions and concerns.
What investigations must be performed prior to surgery?
- Heidelberg University Hospital Departments of Endocrinology, Psychosomatics and Surgery conduct a preliminary examination and must agree on an operation
- Nutritional Counseling (usually two appointments)
- Also carried out: cardiac examination, ultrasound of the neck vessels, 24-hour acidimetry, blood test and smears for drug-resistant bacteria
- If other conditions are present, further investigations may be necessary.
After Bariatric Surgery - Important Notes
- Further follow up visits are recommended within a maximum of six months and then annually, and any time with complaints
- Meal portions must be consistently adjusted after surgery for the long-term. Otherwise there are generally no dietary restrictions. Lifelong vitamin supplementation is often necessary.
- In the initial months post-surgery, many patients report body changes related to rapid weight loss such as: pain, fatigue, feeling cold, dry skin, hair loss, moodiness
- For good cosmetic results, after some time the excess skin and tissues can be removed by a plastic surgeon. For further treatment in Germany we offer this through interdisciplinary collaboration with the Ethianum Clinic in Heidelberg
Treatment inquiry and costs
What is the process? How long is the stay in Germany?
In total, patients should plan for a stay of approximately 8 weeks:
- Preliminary investigations: approximately 2 weeks
- Surgical preparation: 1-2 weeks of protein-rich liquid diet
- Surgery and inpatient stay: approximately 2-5 days
- Ambulatory care (e.g. wound observation, nutritional counseling / adjustment, readjustment of diabetes mellitus): approximately 4 weeks
If complications occur, the patient stay may be longer.
What are the costs of bariatric surgery?
To estimate the costs it's necessary to submit current medical records (no older than 3-6 months), also containing information about possible comorbidities. Based on this information, individualized treatment plan and cost estimate will be created.
How can I send a request?
Please send us, via our international telemedicine portal:
- The completed contact form with important patient information
- a current medical report (in German, English, or Russian)
- Specifications of current height and weight
- If there is a history of other surgery or medical conditions, please send us the most current medical Report.
The International Office will immediately forward the request to an experienced surgeon from the Obesity Center once the completed file with all information has been received. Your documents will be reviewed within a few days and we'll inform you whether we can offer the desired treatment.